Urethral Surgery
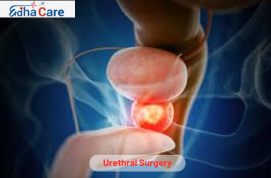
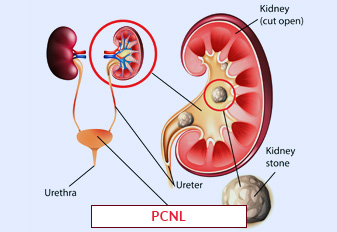
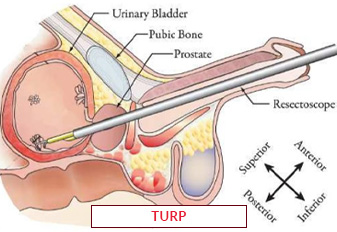
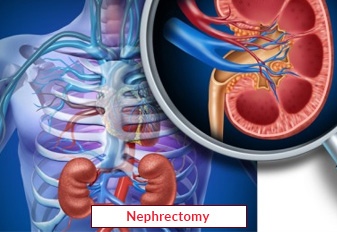
The term "urethral surgery" describes surgical procedures carried out on the urinary tract, which is the tube that exits the body when the urine bladder empties. These surgeries are used to treat a range of urethral diseases, including congenital defects, blockages, strictures (narrowing), and traumas. Urethral dilatation (widening of the urethra), urethrotomy (incision or removal of the scar tissue), and urethroplasty (reconstruction of the urethra) are common forms of urethral procedures. Open surgical approaches or minimally invasive methods like laparoscopic or endoscopic procedures are capable of being utilized to accomplish urethral surgery. Restoring normal urine function, reducing signs, and enhancing the quality of life for those with urethral diseases are the objectives of urethral Stricture surgery.
Book an AppointmentAbout Urethral Surgery
Indications: Direct symptoms are not brought on by urethral surgery. It is, however, used to treat symptoms of diseases impacting the urethra, including difficulties urinating, bleeding in the urine, infections of the urinary tract, and irregular urinary flow.
Causes: A variety of problems affecting the urethra are treated by urethral surgery, such as urethral strictures (narrowing), blockages, trauma, diseases, or congenital defects. Urinary symptoms as well as issues may result from these medical conditions, requiring surgery.
Treatments: Restoring normal urine function, avoiding complications, and reducing the symptoms of urethral disorders are the main objectives of urethral surgery. In order to improve urine flow and general quality of life, surgical operations are performed to fix structural defects, reduce obstructions, or repair broken tissue in the urethra.
Procedure of Urethral Surgery
Preoperative Evaluation: To determine the situation of the urethra and design the surgical method, the patient has a thorough evaluation that involves an overview of their medical records, an examination of the body, and potential imaging scans.
Anesthesia Administration: During the procedure, anesthesia is given to the patient in order to assure their safety and comfort. This could involve either regional or general anesthesia, based on the kind and intricacy of the surgical procedure.
Incision: To reach the affected area, the surgeon creates a small incision at the right place along the path of the urethra. The particular ailment being treated as well as the method of surgery selected will determine the size and placement of the incision.
Correction of Urethral Abnormalities: The surgeon performs the necessary corrective procedures based on the underlying condition. This may involve removing scar tissue, widening the urethra (urethral dilation), reconstructing the urethra (urethroplasty), or repairing injuries or defects.
Closure: After completing the corrective measures, the surgeon closes the incision with sutures or surgical staples to promote proper healing and prevent complications.
Postoperative Care: The patient receives postoperative care instructions, including wound care, pain management, and guidelines for resuming normal activities. Follow-up appointments are scheduled to monitor recovery and assess treatment outcomes.
Recovery and Rehabilitation: The patient undergoes a period of recovery and rehabilitation, during which time they may experience temporary discomfort or urinary symptoms. It's essential to follow postoperative instructions closely and attend all scheduled follow-up appointments to ensure proper healing and optimal outcomes.
Require Assistance?
Get A Quick Callback From Our Healthcare Experts